GCSE | GCSE Maths and English at Grade C (4) or accepted equivalent such as Functional Skills |
Other Admission Requirements | Because nursing and midwifery courses involve clinical placements and strict safeguarding requirements, students must be at least 18 years old at the start of the course to meet professional standards and fully participate in all required activities |
Employment Status | Applicants must be employed full time with a health or social care employer. Evidence of working within care would be beneficial. |
Interview | Applicants meeting the entry requirements will be shortlisted for a values-based interview in line with NMC Standards of Proficiency for Nursing Associates (2024), and the Standards for pre-registration Nursing Associate programmes (2018). |
DBS Check | A DBS Check is required |
Occupational Health | An Occupational Health check is required |
Nursing Associate Higher Apprenticeship FdSc
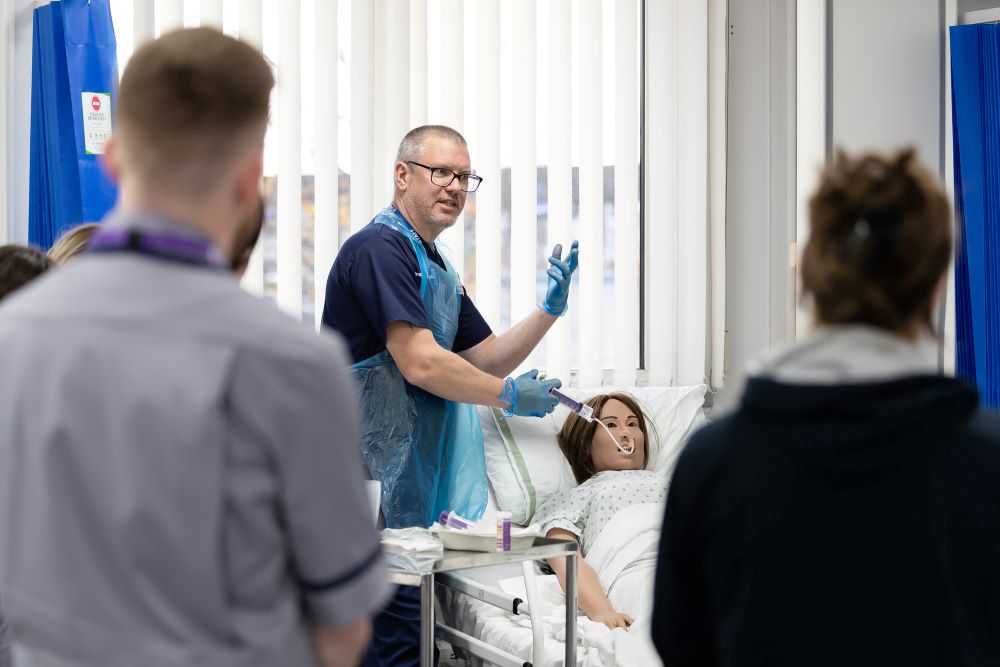
Registered Nursing Associate roles are in a variety of health and social care settings. This Foundation Degree underpins Registered Nursing Associate development, and the course content includes both theory and practice which adhere to the Nursing and Midwifery Council (NMC 2018) Standards of Proficiency for Nursing Associates and the Nursing Associate Higher Apprenticeship Standards (2021).
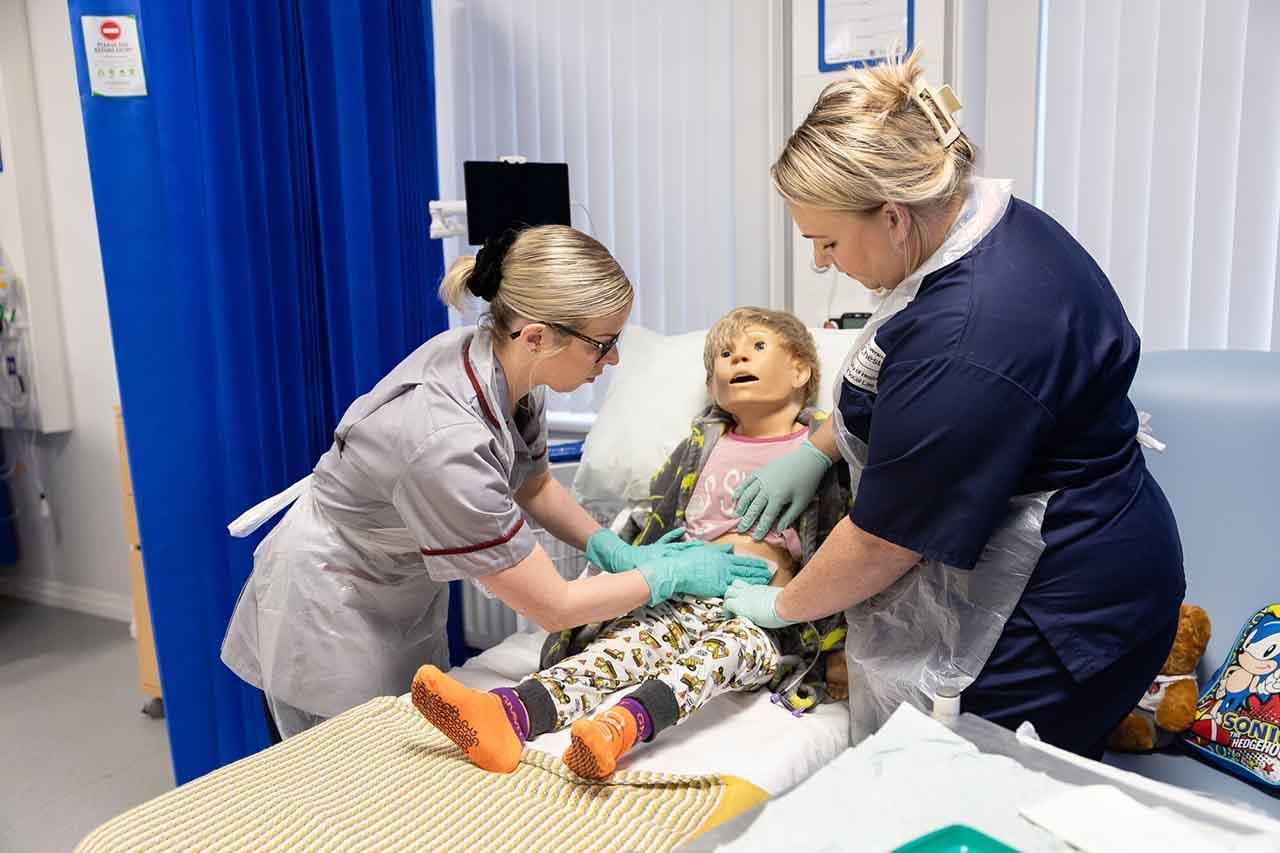
We provide students with amazing subject-specific facilities and a practical approach to learning. Our experienced team of staff work hard to help you realise your potential through a variety of teaching methods, including practice placements.
As an apprentice you will be required by the NMC to complete 460 hours of external practice placements, and you will need to be employed for at least 30 hours per week to be considered full time and be paid at least the minimum wage. However, the course requires you to work 37.5 hours a week. Within your working hours, you will attend one full day at the University of Chester. Your employer will commit to supporting you in practice to achieve work-based learning, development in your role and the application of theory to practice during the remainder of your working week. This will be implemented in varying ways, dependent upon your employing organisation.
Nursing and midwifery courses require clinical placements and strict safeguarding, so students must be at least 18 at the course start to meet professional standards and fully take part in all required activities.

Nursing Associate Higher Apprenticeship FdSc
What You'll Study
Year 1 (Level 4): the following key themes are covered throughout your first year, including: introducing professional and academic lifelong learning; promoting health and preventing ill health across the age continuum; providing and monitoring person centred care; applied anatomy, physiology and integrated pharmacology; practice learning.
The information listed in this section is an overview of the academic content of the course that will take the form of either core or option modules and should be used as a guide. We review the content of our courses regularly, making changes where necessary to improve your experience and graduate prospects. If during a review process, course content is significantly changed, we will contact you to notify you of these changes if you receive an offer from us.
In Year 2 (Level 5), you will continue to study the ethos of person-centred care as well as developing your skills to become a registered practitioner, including: enhancing professional and academic learning; medicines management; working in teams; practice learning; integrated care; trans-professional research and innovation.
The information listed in this section is an overview of the academic content of the course that will take the form of either core or option modules and should be used as a guide. We review the content of our courses regularly, making changes where necessary to improve your experience and graduate prospects. If during a review process, course content is significantly changed, we will contact you to notify you of these changes if you receive an offer from us.

How we teach at the University of Chester
You will experience a variety of teaching and learning methods designed to facilitate achievement of learning outcomes and to foster your development. These include:
- formal group-based learning sessions
- e-learning/blended learning opportunities
- learning through practice
- private directed study.
Assessment methods include:
- reflective portfolios
- learning logs
- practical examinations
- practice-based assessment
- case studies
- assignments.
Your Future Career
Job Prospects
On successful completion of the course, you will be able to register with the Nursing and Midwifery Council as a registered practitioner. It is anticipated you will be employed in any one of a range of health care settings such as:
- Hospitals
- Community care
- Primary care
- Care homes
- Mental health and learning disability services
- Hospices
- Private health care
- Education institutions
Careers Service
The University has an award-winning Careers and Employability service which provides a variety of employability-enhancing experiences; through the curriculum, through employer contact, tailored group sessions, individual information, advice and guidance.
Careers and Employability aims to deliver a service which is inclusive, impartial, welcoming, informed and tailored to your personal goals and aspirations, to enable you to develop as an individual and contribute to the business and community in which you will live and work.
We are here to help you plan your future, make the most of your time at University and to enhance your employability. We provide access to part-time jobs, extra-curricular employability-enhancing workshops and offer practical one-to-one help with career planning, including help with CVs, applications and mock interviews. We also deliver group sessions on career planning within each course and we have a wide range of extensive information covering graduate jobs and postgraduate study.
Beyond the Classroom
On this apprenticeship, you’ll spend time out on placement where you’ll apply what you have learnt to real scenarios in healthcare settings, giving you genuine experience and insight that will prepare you for your future career.
Entry Requirements
Fees and Funding
£9,790 per year for a full-time course (2026/27)
The full-time tuition fees for Home students entering in 2026/27 are £9,790 a year, or £1,590 per 20-credit module for part-time study.
You can find more information about undergraduate fees on our Fees and Finance pages.
Students from the UK, Isle of Man, Guernsey, Jersey and the Republic of Ireland are treated as Home students for tuition fee purposes.
Students from countries in the European Economic Area and the EU will pay International Tuition Fees.
Students who have been granted Settled Status may be eligible for Home Fee Status and if eligible will be able to apply for Tuition Fee Loans and Maintenance Loans.
Students who have been granted Pre-settled Status may be eligible for Home Fee Status and if eligible will be able to apply for Tuition Fee Loans.